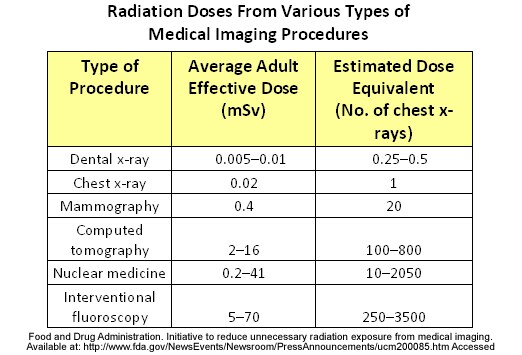
Currently, Medicare pays approximately a national average of $24,000 for a cochlear implant, but $0 for hearing aids (Table 1). Let's examine this coverage disparity from scientific, regulatory, and political viewpoints.

First, to be covered by Medicare, a device must provide a health benefit and “be determined to be reasonable and necessary for the diagnosis or treatment of an illness or injury or to improve the functioning of a malformed body member” (Social Security Act
http://bit.ly/2bgSJHc).
As early as October 1986, cochlear implants, both 3M/House single-channel and Nucleus-22 devices, were covered for adult Medicare beneficiaries. This was supported by a 44-page report on scientific and clinical evidence from the Office of Health Technology Assessment (OHTA), a federal agency that made Medicare policy recommendations at the time (Feigenbaum. NCHSR, 1986
http://bit.ly/2bgVhW9). The 1986 report determined that cochlear implants restored sound detection, improved voice modulation and lip-reading, and, in some patients, provided a considerable degree of open-set speech recognition.
In 1992, Medicare coverage of the cochlear implant was extended to children. In 2005, the Centers for Medicare and Medicaid Services (CMS) markedly expanded the audiological criterion to include individuals who received a pre-implant score of ≤40 percent open-set sentence recognition under the best-aided listening condition (CAG-00107N
http://go.cms.gov/2bgTiB0).
Today, Medicare not only covers the cochlear implant, but also its accessories such as microphones and batteries. The surgery may include additional coverage from the use of operating microscope to intra-surgical monitoring.
The OHTA and CMS guidelines relied heavily on peer-reviewed publications; to a lesser extent, on data submitted by the manufacturers to the Food & Drug Administration (FDA) and on professional society position statements; and the least extent, on expert opinions. For example, the CMS responded to three commentators who provided solid but unpublished data that they “encourage parties with such data to pursue publication, and thereby enlarge the pool of published evidence.”
Apparently, the CMS has determined that the published evidence on the health benefits of hearing aids is inadequate, and that, accordingly, hearing aids do not merit any coverage.
http://journals.lww.com/thehearingjourn ... ot.10.aspx